Atopic eczema and allergy tests
The immune system of the body is part of its defence against disease. It can neutralise pathogens, or threats to health, such as viruses and bacteria. Such outside threats are called antigens, against which the immune system reacts by producing protective antibodies.
An allergy is an immune reaction to something that is normally harmless. The antigen is then called an allergen. The allergy antibody is called immunoglobulin E (IgE). The allergen-antibody reaction causes a tissue reaction called inflammation. The severity of such inflammation ranges from being uncomfortable to dangerous.
Atopy is a descriptive word meaning “strange disease”. It refers to being prone to getting asthma, eczema, and hay fever. It is strongly associated with developing allergies, and seems to run in families. Although atopy is sometimes regarded as the ability to produce particular antibodies to certain allergens, a small but significant percentage of people with typical atopic eczema do not show this immune reaction, at least using the tests currently available. Therefore atopic eczema remains a clinical diagnosis, regardless of such tests.
For atopic eczema there are three types of allergy test commonly referred to: patch tests, prick tests and blood tests.
- Patch tests
Atopic patch tests are chiefly useful for identifying allergy to substances that the skin has contact with. These range from metal such as nickel - present in a wide range of things found in every home - to preservatives and perfumes in creams, and on to the topical treatment itself. Lanolin, in wool fat, used in some moisturisers, can provoke allergies in some. If it does, it needs avoiding.
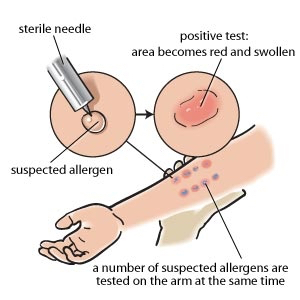
- Prick tests
Small amounts of suspected allergens, for example pollen, grass, house dust mite, or peanuts - or extracts from them - are injected into the skin. If there is an allergy it usually shows with a red inflammatory reaction within thirty minutes.
- Blood tests
With a simple blood test, ninety per cent of people with atopic eczema have a raised IgE level. This is the general type of antibody associated with allergies. The total IgE level, and the specific antibody level to particular antigens, can be measured - without any exposure to any suspected allergen. This can be helpful in planning treatment: see below.
Case report:
A sixty-two year man with life-long asthma, had had eczema previously as a baby. It cleared up then, only to return when he was 55, when it became severe, and resistant to conventional treatment. He was therefore treated with immunosuppressant drugs - azathioprine, and cyclosporin - which seemed helpful, but caused important side effects. Review with a blood test then revealed an unsuspected very strong allergy to house dust mite: when he followed advice about house cleaning and new bedding, he was delighted to report a marked improvement in his eczema.
What has your experience been?
